What Is Gum Recession?
Gum recession happens when the gum tissue around a tooth pulls back or wears away, exposing the root of the tooth that is normally hidden beneath the gum line. You might notice your teeth looking longer than they used to, or you might feel a notch near the gum line with your fingernail.
Recession is very common. Research shows that more than half of adults over age 30 have some degree of gum recession, and that number rises to over 80% of adults over age 65. While many people think of it as a cosmetic issue, recession can lead to real health problems if left untreated, including tooth sensitivity, cavities on the root surface, gum infections, ongoing bone loss, and in severe cases, tooth loss.
Your Gum Anatomy: Why It Matters
To understand recession, it helps to know a little about the different types of gum tissue. Your gums aren't all the same; there are three distinct zones, each with a different job.
The Three Zones
Free gingiva (the collar): This is the strip of gum tissue closest to the crown of your tooth. It forms a small cuff around each tooth, creating a shallow pocket called the sulcus. In a healthy mouth, this pocket measures 1–3 mm deep. That's the number your hygienist calls out during your exam.
Attached gingiva (the seal): This is the firm, pink gum tissue that is physically bound to the root of your tooth and the underlying bone. It's the most important part of the system because it forms a tight seal that keeps bacteria from getting down along the root and into the deeper tissues. Think of it like the gasket in a pressure cooker: without it, nothing stays sealed.
Alveolar mucosa (the lining): This is the loose, darker tissue below the attached gingiva. It's thin, stretchy, and mobile; good for lining the inside of your mouth, but completely unable to form a seal against your tooth or bone. When recession eliminates the attached gingiva and all that remains at the gum line is this loose lining tissue, the protective barrier is lost.
The Key Number: 2 mm
Research has shown that a minimum of about 2 mm of keratinized tissue (the free gingiva plus attached gingiva combined) is needed to protect your tooth and keep the gum stable. Below that threshold, the gum loses its ability to seal out bacteria and resist the forces of daily life: eating, talking, and even facial expressions.
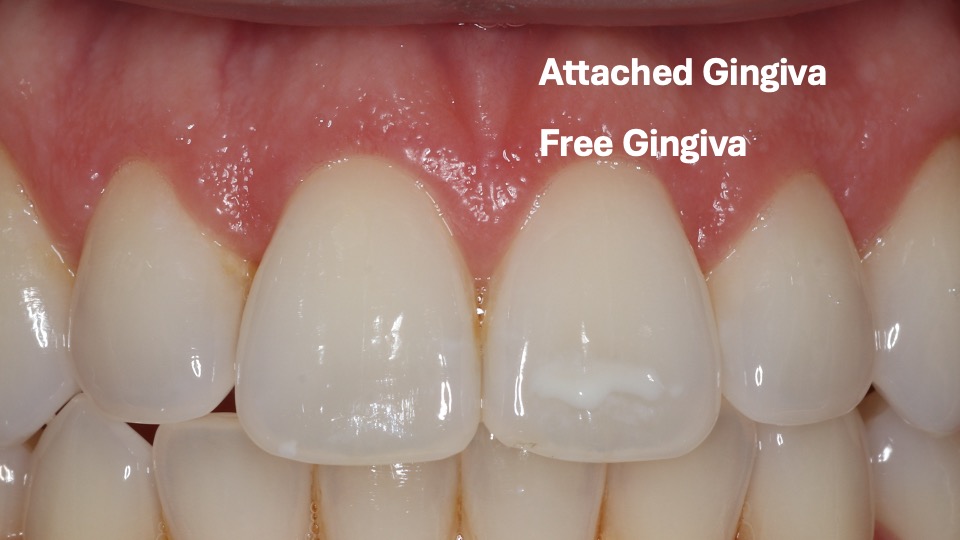
This patient has healthy thick gum tissue. The free gingiva is the cuff surrounding the tooth and the attached gingiva is the thick tissue attached to the bone. Both of these are made of keratinized tissue.
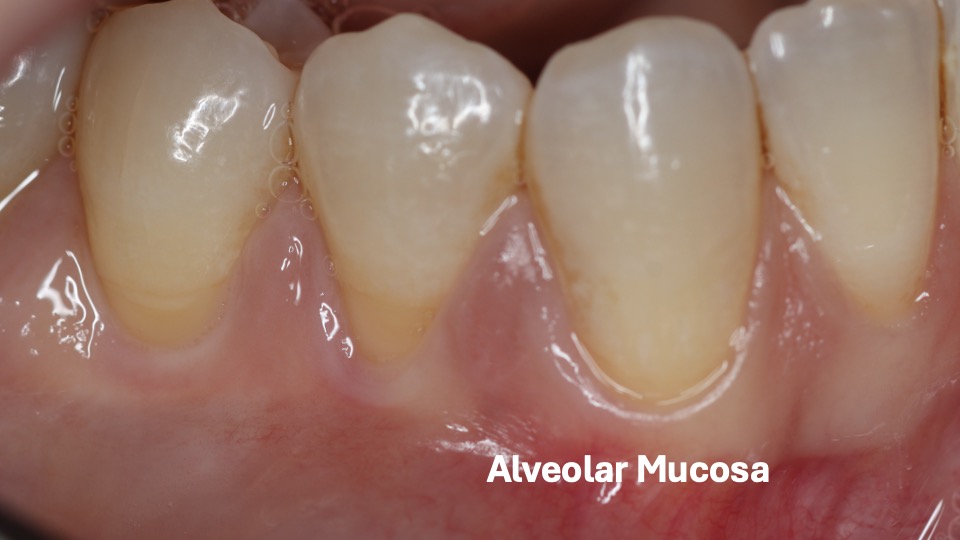
This patient is lacking all keratinized tissue. They only have thin alveolar mucosa surrounding their teeth which is leading to both recession and bone loss.
Gum Tissue Around Implants
If you have dental implants, the gum tissue around them works similarly but has one important difference: the gum cannot form the same strong fiber attachment to an implant that it can to a natural tooth. The tissue can seal against the bone near the implant, but it doesn't actually attach to the implant surface itself. This means implants may need even more protective gum tissue than natural teeth to stay healthy.
Newer implant surface technologies (such as the Xeal surface on Nobel Biocare implants) have been designed to improve how tissue bonds to the implant collar, and research shows they do enhance the seal compared to older designs. However, the fundamental limitation remains: the connection between gum and implant is not as strong as the connection between gum and tooth.
Why This Matters for Your Implants
If Dr. Yant recommends gum grafting around your implants, it's because the absence of attached tissue, even if there appears to be a visible band of gum, means there's no functional seal protecting the implant from bacteria. Grafting creates that seal and can protect your implant investment for the long term.
What Causes Gum Recession?
Recession rarely has a single cause. In most patients, it's a combination of factors working together. Here are the four main categories:
1. Tooth Position
If a tooth, or more specifically, its root, sits outside the protective bony housing (the jawbone), the overlying gum is thin and vulnerable. This can happen naturally (some people are simply born with teeth in this position) or as a result of orthodontic treatment that moves teeth beyond the bone envelope. Orthodontically-related recession typically shows up within 3 years of finishing treatment and is more common in patients over 16 years of age, when the gum tissue is thinner and less adaptable than in younger patients.
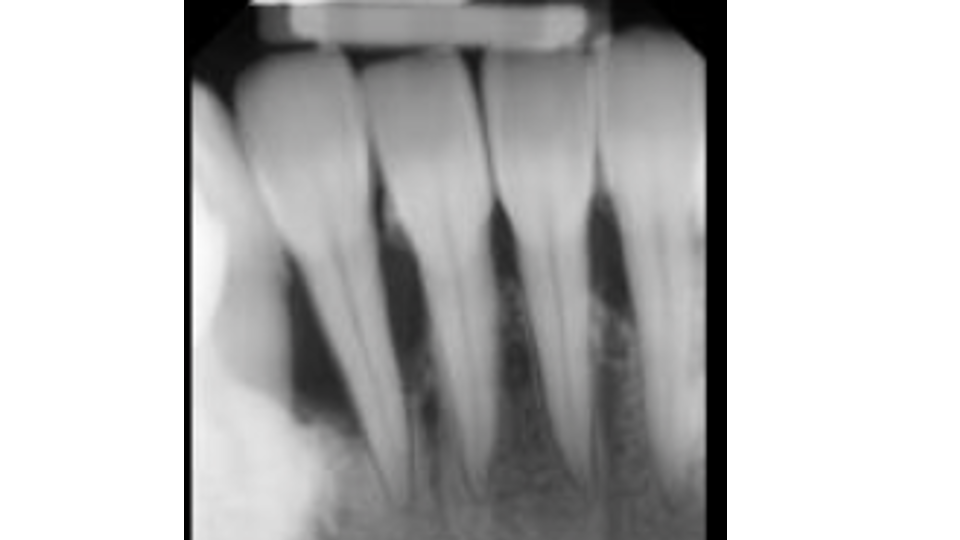
2. Gum Disease (Periodontitis)
Gum disease is a bacterial infection that destroys the bone and tissue supporting your teeth. In patients with thin gum tissue, gum disease directly causes recession as the bone is destroyed. In patients with thicker tissue, recession can sometimes appear after gum disease treatment, because the swollen, infected tissue shrinks back to the level of the bone once the infection is cleaned out. This isn't a failure of treatment; it's actually a sign that the inflammation has resolved.
3. Aggressive Tooth Brushing
Brushing too hard, using a medium- or hard-bristled brush, or scrubbing side to side (rather than using a gentle circular technique) can physically wear away gum tissue over time. A telltale sign is the presence of V-shaped notches at the gum line where the tooth surface has been abraded along with the gum. These are called abfraction or non-carious cervical lesions. If Dr. Yant sees these notches, it's a strong clue that brushing technique is contributing to the recession.
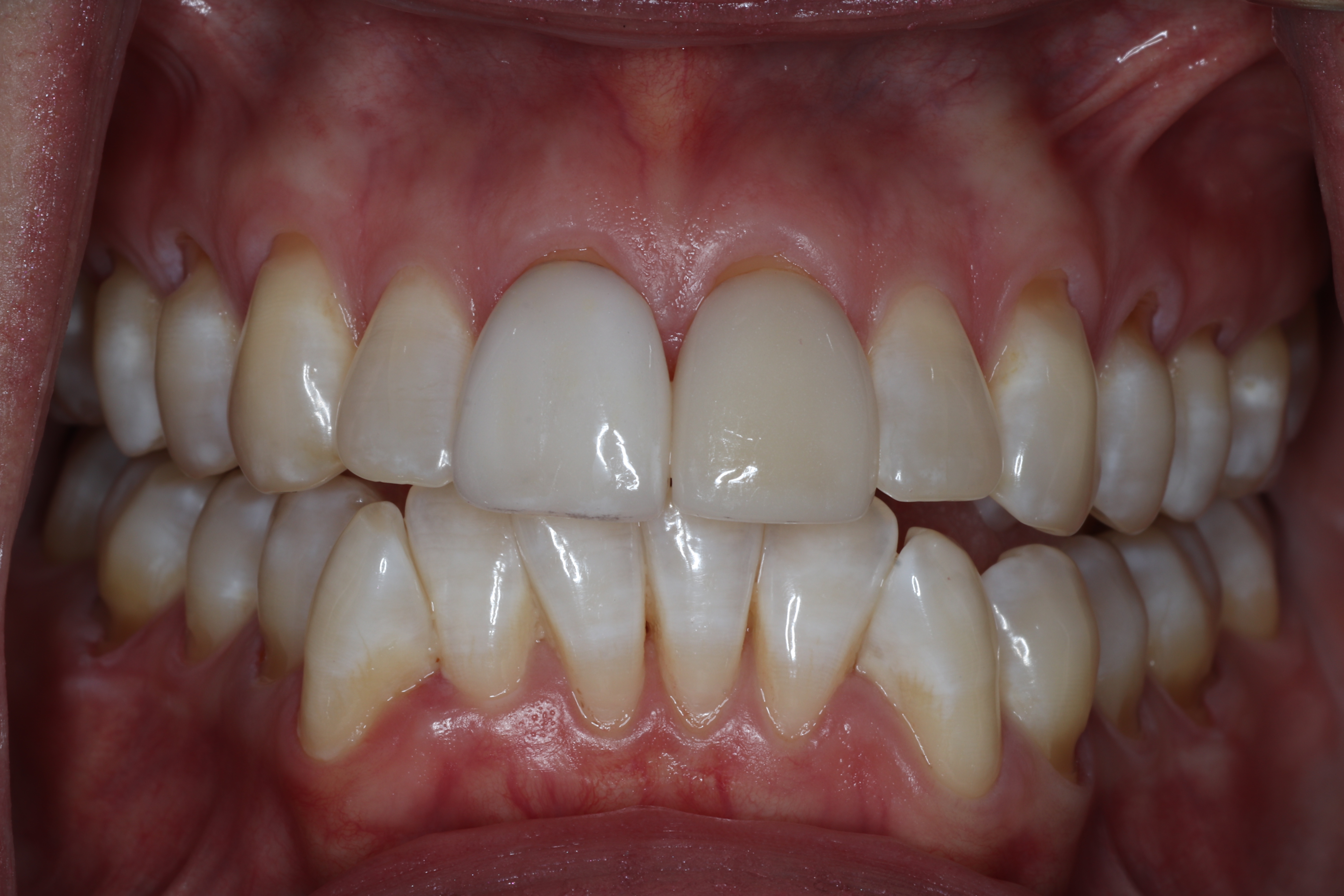
4. Not Enough Protective Gum Tissue
This is the most important cause to understand because it's the one that most often requires surgical treatment. When there isn't enough keratinized tissue (less than 2 mm), and especially when the attached gingiva is missing, two things happen:
The "vacuum" effect: Without a seal between the gum and the tooth, everyday movements like eating, talking, and facial expressions cause the loose tissue to pull away from the tooth. This creates a pumping action that draws bacteria and debris down along the root surface. If there's a strong muscle or lip attachment (called a frenum) pulling on the tissue in that area, the pumping effect is even worse, significantly increasing the risk of gum infections and ongoing recession.
Inflammation burns through thin tissue: When bacteria accumulate at the gum line and the gum tissue is thin and unprotected, the resulting inflammation can penetrate the full thickness of the tissue and destroy the collagen that holds it together. This causes the tissue to recede further, exposing more root, which attracts more bacteria, creating a vicious cycle.
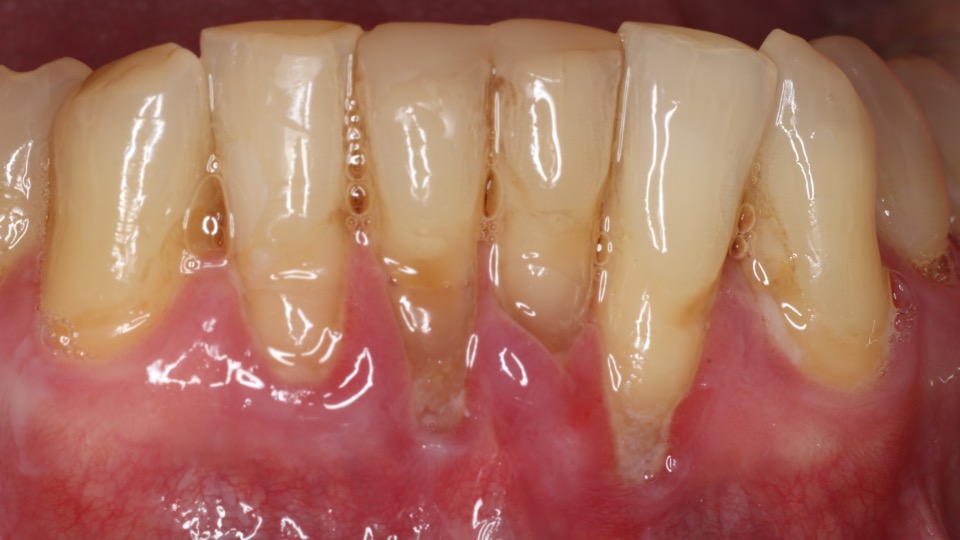
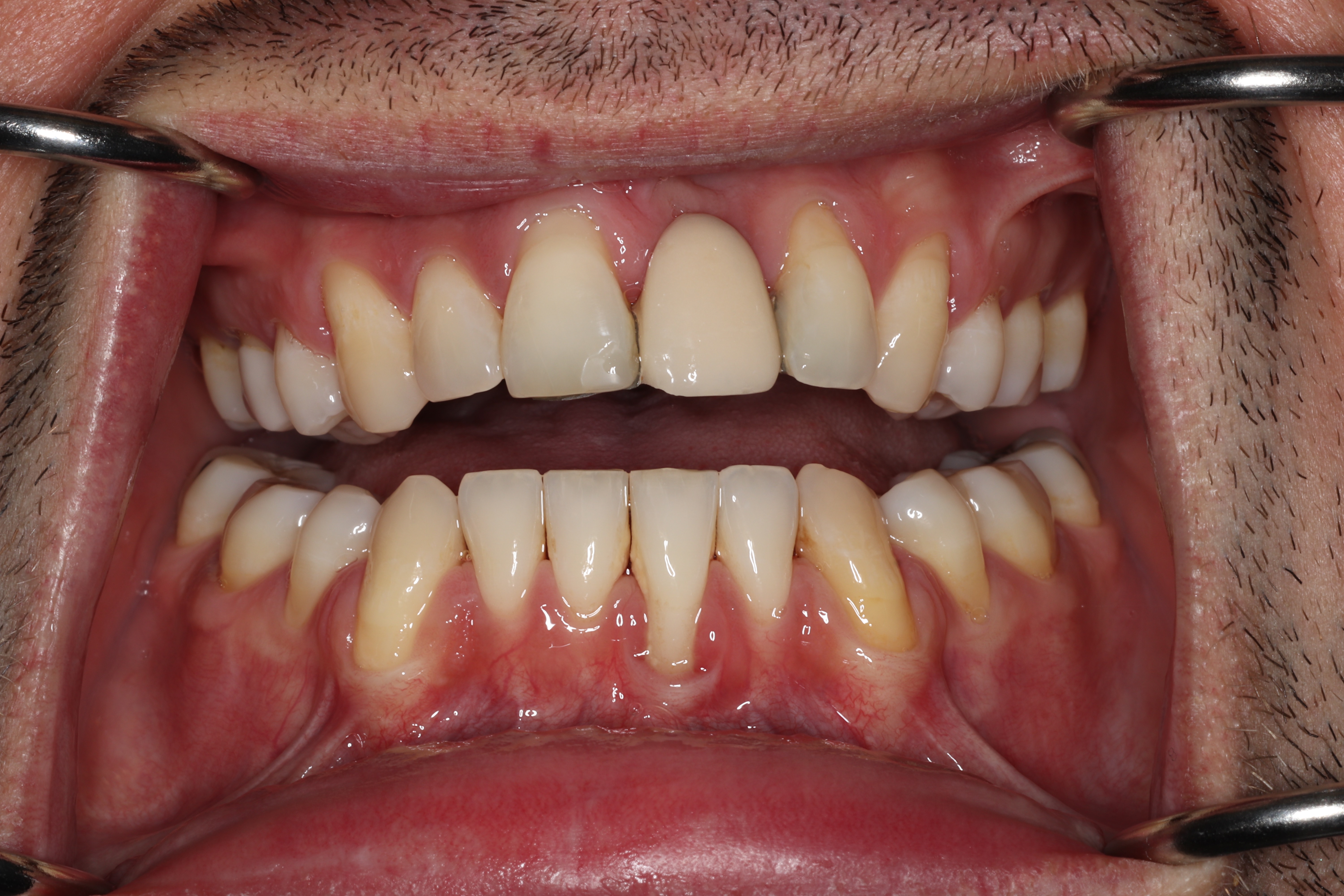
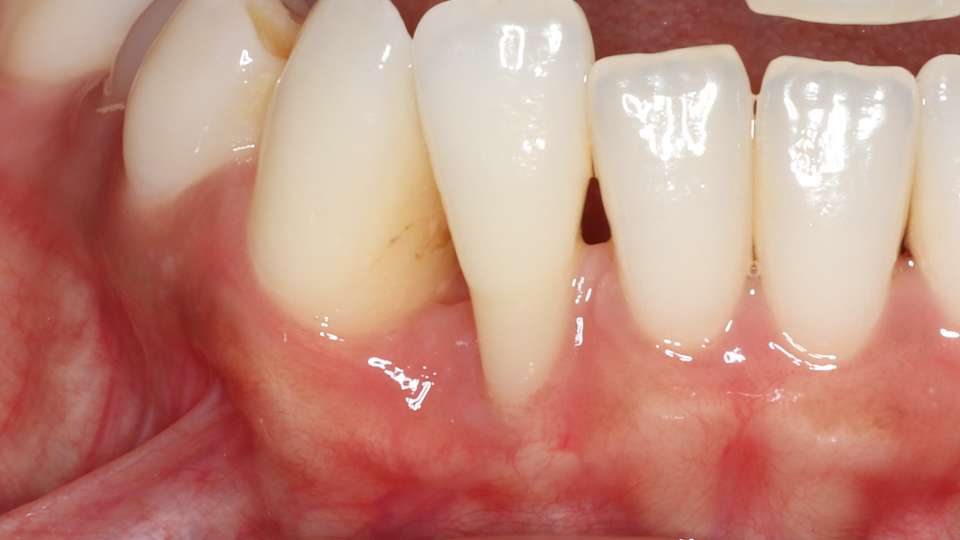
Take a closer look at the difference between the two areas in this patient's mouth. The teeth surrounded by thick, firmly attached protective tissue show no plaque buildup, no inflammation, and stable, healthy gum levels. In contrast, the sites that lack this protective tissue are visibly inflamed and collecting bacteria along the gumline, which is driving progressive recession. Without intervention to rebuild that protective barrier through grafting, the affected teeth would continue to lose gum tissue and bone support over time, ultimately putting them at risk of being lost entirely.
What Happens If Recession Is Left Untreated?
- Gum infections (abscesses): Without attached tissue forming a seal, bacteria have a direct pathway into the deeper tissues around your tooth or implant. This can lead to painful abscesses, especially when a strong muscle pull keeps opening the tissue like a door.
- Ongoing bone loss: Bacteria that migrate down an unsealed root surface can reach the bone supporting your tooth. When that happens, your body's inflammatory response actually resorbs (destroys) the bone to try to maintain distance from the bacteria. This creates a cycle: bone loss exposes more root, which allows more bacteria, which causes more bone loss.
- Root cavities: The root surface is softer and more porous than the enamel crown of your tooth, making it much more vulnerable to decay. Root cavities can progress quickly and are harder to treat than regular cavities.
- Tooth sensitivity: When root surface is exposed, tiny tubes in the dentin (called dentinal tubules) are open to the outside. Temperature changes, cold air, sweet or sour foods, and even touching the area can trigger sharp, shooting pain.
- Cosmetic concerns: Recession in the front teeth causes visible root exposure, teeth that appear longer than normal, color differences between the white enamel and the yellower root, and gaps between teeth at the gum line.
When Is Treatment Needed?
Dr. Yant will recommend gum grafting surgery when one or more of these situations applies:
- Your protective gum tissue is less than 2 mm wide. Below this threshold, the gum can no longer protect your tooth from bacteria or withstand normal daily forces.
- You're planning orthodontic treatment. If you have thin gum tissue and your orthodontist plans to move your teeth outward, pre-treatment grafting can prevent recession from developing during or after braces or aligners. This is especially important for adult patients.
- The recession makes it impossible to keep the area clean. When the gum line is significantly lower than neighboring teeth, or when brushing is too painful because the protective tissue is gone, surgery can restore a gum architecture you can actually maintain.
- Your implants lack attached tissue. Because implant gum tissue can't form a true attachment to the implant surface, grafting is especially important to create the seal that protects your implant from infection and bone loss.
- You want to address cosmetic root exposure. When recession is in your smile zone and the anatomy is favorable for root coverage, Dr. Yant can often cover the exposed root and restore a natural-looking gum line.
When Grafting Is NOT Needed
If you have recession but still have at least 2 mm of protective keratinized tissue, surgery is usually not necessary. Instead, Dr. Yant will focus on correcting the underlying cause: modifying your brushing technique, completing gum disease treatment, or monitoring after orthodontic treatment.
Here's the most important takeaway: in most cases where recession is caused only by tooth position, gum disease, or brushing habits, and where you still have enough protective gum tissue remaining, you do NOT need surgery. Changing your brushing technique or completing gum disease treatment is enough. It's primarily when the protective tissue is deficient that grafting becomes necessary to prevent further damage.
Ready to Learn About Treatment Options?
If you or Dr. Yant have determined that gum grafting is needed, learn what to expect from the procedure, recovery, and results in our comprehensive treatment guide: Soft Tissue Grafting: Treatment for Gum Recession.
Frequently Asked Questions
What causes gum recession?
Gum recession can be caused by periodontal disease, aggressive brushing with a hard-bristled toothbrush, genetics, teeth grinding or clenching, tobacco use (including smoking, dip, and Zyn pouches), misaligned teeth, or hormonal changes. In many cases, multiple factors contribute at the same time.
Can receding gums grow back?
No. Once gum tissue has receded, it does not grow back on its own. However, soft tissue grafting can restore gum coverage over exposed roots, reduce sensitivity, and protect the teeth from further damage. Early intervention produces the best results.
How do I know if my gums are receding?
Common signs include teeth that appear longer than they used to, a notch you can feel near the gum line, increased sensitivity to hot or cold, and visible root surfaces that appear darker or more yellow than the crown of the tooth. Your dentist can measure recession during a routine exam.
Is gum recession serious?
Yes. Gum recession exposes the root surface of the tooth, which is softer than enamel and more vulnerable to decay. Without the protective gum tissue, the underlying bone is also at risk of loss. Untreated recession can lead to sensitivity, root cavities, and eventually tooth loss.
Does brushing too hard cause gum recession?
Yes. Aggressive brushing is one of the most common causes of gum recession, especially when using a hard-bristled toothbrush. Using a soft or ultra-soft toothbrush with gentle circular motions protects the gum tissue while still effectively cleaning the teeth.
Can Zyn pouches or dip cause gum recession?
Yes. Oral tobacco products including Zyn nicotine pouches, dip, and chewing tobacco cause direct chemical and mechanical irritation to the gum tissue where they are placed. This irritation leads to gum recession, and the damage worsens with continued use. Stopping oral tobacco is essential to preventing further recession.
Sources
This guide is based on peer-reviewed research published in leading dental and medical journals, the same sources used in periodontal residency training programs.
- American Academy of Periodontology. (1996). Glossary of periodontal terms (3rd ed.). Chicago: AAP.
- Cortellini, P., & Bissada, N. F. (2018). Mucogingival conditions in the natural dentition. Journal of Periodontology, 89(Suppl. 1), S204–S213.
- Joss-Vassalli, I., et al. (2010). Orthodontic therapy and gingival recession: a systematic review. The Angle Orthodontist, 80(1), 139–145.
- Kassab, M. M., & Cohen, R. E. (2003). The etiology and prevalence of gingival recession. Journal of the American Dental Association, 134(2), 220–225.
- Kim, D. M., & Zucchelli, G. (2020). Mucogingival considerations in implant therapy. In Lindhe's Clinical Periodontology (7th ed.). Wiley-Blackwell.
- Lekholm, U., et al. (2021). TiUltra surface and Xeal mucosal connection: a narrative review. Clinical Oral Implants Research, 32(Suppl. 21), 19–28.
- Rajapakse, P. S., et al. (2007). Does tooth brushing influence the development and progression of non-inflammatory gingival recession? Journal of Clinical Periodontology, 34(12), 1046–1061.
- Serino, G., et al. (1994). The prevalence and distribution of gingival recession. Journal of Clinical Periodontology, 21(1), 57–63.
- Wennström, J. L. (1987). Lack of association between width of attached gingiva and development of recession. Journal of Clinical Periodontology, 14(3), 181–184.
Questions About Your Periodontal Health?
If you have concerns about your gum health or would like to learn more about any of the topics discussed in this article, we are here to help.